Sebastian Sanchez's sudden illness revealed one of the fastest-growing cancers. Through seamless collaboration across specialties, UConn Health's academic medical center delivered the complex, time-sensitive care needed to save his life

Sebastian Sanchez and Dr. Kapil Meleveedu are all smiles at a follow up appointment.
Just weeks before his life changed, Sebastian Sanchez was doing everything right.

At 23, he was active, health-conscious, and working long hours in a kitchen where he had just begun to discover a passion for cooking. His days were structured around work, workouts, and routine.
Then, in early December 2023, his body sent a signal he couldn't ignore.
What felt like a cold quickly escalated into relentless nausea, vomiting, and crushing fatigue. Sleep offered no relief. Then came the pain, deep, tightening pressure in his abdomen and chest.
"It felt like someone was squeezing under my ribs," Sanchez says. "Then it moved higher, it felt like something was grabbing near my heart."

Within days, his condition deteriorated to the point where even standing was exhausting. He finally reached out and asked his sister, Andrea, to take him to the emergency department at UConn John Dempsey Hospital, still unsure of what they would find.
By the early hours of the morning, Sebastian and Andrea were facing devastating news: what appeared to be cancer.
Andrea was the one who had to leave the hospital and tell their parents, shouldering the weight of that moment while remaining a steady presence for her brother.
"I was more worried about how this would affect my family than myself," Sanchez says.
He was soon diagnosed with Burkitt's lymphoma, one of the fastest-growing human tumors, an aggressive cancer of the lymphatic system that requires immediate, highly specialized treatment. Burkitt's lymphoma is known for how quickly it progresses and how quickly treatment must begin.
"Conditions like Sanchez's don't give you the luxury of time," explains Dr. Kapil Meleveedu, director of Blood and Marrow Transplantation at UConn Health Carole and Ray Neag Comprehensive Cancer Center, who led Sebastian's oncology care. "You often need to begin treatment even before you have every answer, because the disease can advance rapidly."
His case triggered an immediate multidisciplinary response from the team at UConn Health. Oncology, hematopathology, gastroenterology, internal medicine, interventional radiology, general surgery, neurosurgery, and critical care teams worked simultaneously to confirm the diagnosis, stage the disease and stabilize his rapidly changing condition.
Advanced imaging revealed extensive lymph node involvement, including areas that were begging to compromise surrounding organs and at the base of his skull, explaining the intense pain Sanchez had been experiencing.
But before chemotherapy could begin, a life-threatening complication emerged.
One of those lymph nodes compressed part of his intestine, ultimately leading to a perforation of his intestine, requiring emergency surgery.
From a clinical standpoint, the situation became even more complex.
"That was a pivotal moment," Meleveedu says. "We had a cancer that needed immediate treatment, but we also had a surgical emergency that had to be addressed first. Managing both simultaneously is incredibly complex. Avoiding either was not an option."
The care team faced a series of high-stakes decisions, balancing competing priorities across multiple specialties. Through in‑depth multidisciplinary discussions – bringing together oncology, surgery, and neurosurgery they weighed the risks and benefits of each step and aligned on a coordinated plan. Dr. Alyson Cunningham and her general surgical team urgently intervened and offered the lifesaving surgery. Meleveedu and the hematology oncology team instituted the safest way to give multi-agent systemic chemotherapy ensuring safety guardrails for someone who just had a major surgery. Dr. Ian McNeill, neurosurgeon at the UConn Health Brain and Spine Institute, placed a scalp port (called an Ommaya reservoir) to deliver chemotherapy directly into his cerebrospinal fluid.
That level of alignment, Meleveedu noted, is a hallmark of academic medicine.
"When care is this complex, collaboration isn't optional, it's essential," he says. "We rely on a multidisciplinary approach with all contributing their expertise to one unified plan."
Sanchez's journey did not get easier after the first surgery. In total, he underwent three emergency procedures. After the initial perforation, scar tissue caused a blockage in his intestine. Weeks later, his intestines became twisted and needed to be surgically corrected. He had multiple complications from wound healing and intractable pain, protein calorie malnutrition infections, fever, and arrythmias, requiring multiple hospitalizations and different specialists' care over subsequent months.
He also required an ileostomy, a temporary but life-altering adjustment that would remain for nearly a year.
"That was the hardest part for me," he says. "More than the chemo or anything, it was the fear that I might not be able to get that reversed."
For someone who had lived an active, fitness-focused lifestyle, the adjustment was deeply personal. It affected how he moved, how he saw himself and how he engaged with the world.
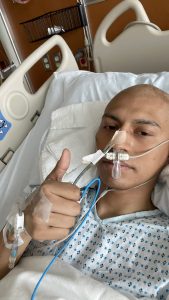
Throughout it all, his care team remained focused on not just treating his cancer, but on preserving his long-term quality of life.
His sister Andrea also played a pivotal role in his recovery. Whether sitting at his bedside, speaking with clinicians, or simply being present during long, uncertain days, her role extended far beyond that of a visitor.
For Meleveedu, that presence is more than emotional support – it's clinically meaningful.
"Caregivers like Andrea are part of the care team," he says. "They help patients stay grounded, ensure continuity in communication, and often recognize subtle changes that can be important. That partnership improves care."
Over months of inpatient and outpatient treatment, Sanchez's condition began to improve. Scans showed progress. Tumors shrank. His body responded.
"The doctors and nurses were always encouraging me to stay positive," he recalls. "They were always checking in to see what I needed, and I didn't feel like I was just a patient."
That human connection combined with clinical excellence helped carry him through.
By summer, Sanchez was strong enough to return to work and slowly rebuilt his endurance, working his way back to running, lifting weights, and living the life he had put on hold.
And eventually after a year, he reached a milestone he had been waiting for: the reversal of his ileostomy.
Today, Sanchez is cancer-free, with an excellent prognosis.

His prognosis is excellent and he continues with routine follow-up appointments, but his focus has shifted.
This experience has changed him. "It made me realize I have a second chance," he says. "I don't want to waste it."
But he's quick to point out that this wasn't something he went through alone
"This wasn't just me," he says. "It was my family, my sister, and the entire team, from the front desk to the last nurse who walked me out, everyone was incredible."
For him, UConn Health became more than a hospital. It became a second home.
And for Meleveedu, stories like Sanchez's reflect what academic medicine is all about.
"The best outcomes happen when exceptional clinical care is paired with strong support systems," he says. "Sebastian had both."






